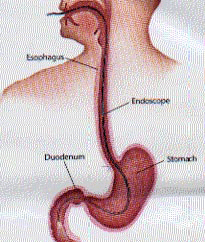
Sometimes referred to as upper GI endoscopy, esophagogastroduodenoscopy (EGD), or panendoscopy, the upper endoscopy occurs when a physician needs to appraise the lining of the upper part of the patient’s GI tract; including the esophagus, stomach, and duodenum. During an upper endoscopy, a small flexible tube-shaped camera called an endoscope will examine the upper part of the gastrointestinal tract, and feed images onto a monitor for the doctor.
Why Might I Need an Upper Endoscopy?
What to Expect During the Procedure
Why Might I Need an Upper Endoscopy?
An upper endoscopy can serve many purposes, including diagnosing symptoms of chronic upper abdominal pain, upset stomach, vomiting, or difficulty swallowing. The benefit of the procedure is that it can be used to assist in treating many different conditions. For example, instruments can be passed through the endoscope to stretch or dilate a narrow area of the GI tract, to remove polyps, or treat abnormalities; all without causing the patient any considerable discomfort. Upper Endoscopy is also known to be more accurate than X-rays when being used for diagnosing ulcers, tumors, and pinpointing the cause of bleeding in the upper GI tract. This procedure may also be used to perform a cytology test, in which a small brush is used to collect cells for analysis; similar to a biopsy.
Preparing for the Procedure
Preparation for the EGD is relatively simple: the procedure requires an empty stomach, so there should be no ingestion of food or drink (including water) approximately six hours before the exam. Timing can vary for certain patients, so a doctor will follow up with further detail when it is time to start fasting.
Depending on the procedure that is being performed, there are several necessary preparations, which a doctor or nurse will cover in further detail before the appointment. Some patients may need to prepare for a Fructose Intolerance Breath Test, while others will prepare for the esophagogastroduodenoscopy, commonly known as EGD.
Most medications can be taken as normal, but some will interfere with the upper endoscopy preparation or examination. Before the procedure, always be sure to mention any medications that are being administered, as the dosage could be changed temporarily for patient safety. Also mention any existing medical conditions or allergies, as it could significantly alter care. Aspirin products or antiplatelet agents, arthritis medication, anticoagulants (such as warfarin or heparin), clopidogrel, insulin, or iron products are cause for particular concern.
What to Expect During the Procedure
Before an upper endoscopy, a physician may spray the throat with a local anesthetic or offer a sedative to help the patient relax. The patient will be in a light sleep due to medication administered intravenously by an anesthesiologist and will have to lay on their side before they are completely asleep.
During an upper endoscopy, the doctor will enter an endoscope into the mouth, through the esophagus, and into the stomach, which then leads to the duodenum. This tool will not impede on the patient’s breathing or cause any discomfort.
During the procedure, the physician may choose to take a tissue sample, otherwise known as a biopsy, of any area that he or she feels may need further examination. These samples help the physician determine if the cells tissue is benign or malignant (cancerous). However, biopsies are not always ordered to test for cancerous cells, and should not automatically cause concern. For example, polyps, though typically benign, are commonly removed during an upper endoscopy. Physicians may also order a biopsy to diagnose Helicobacter pylori, which is a type of bacterium that will cause ulcers.
After the Procedure
After an upper endoscopy is completed, the patient will wake up within a few minutes. There will then be a period of time where the patient is monitored until most of the anesthesia has worn off, and then they can be discharged unless a physician instructs otherwise. The physician who performed the procedure will explain the results, and let the patient know if there were any biopsies performed; in which case, there will likely be a delay in the results as the tissues are tested. If sedatives were administered, someone might have to drive the patient home and stay with them. Additionally, the throat may feel some initial irritation, and the stomach may feel bloated due to the introduction of additional air during the exam. Patients may eat directly after the procedure unless their doctor gives other instructions.
Is an Upper Endoscopy Safe?
Complications during an upper endoscopy are rare, primarily when the procedure is performed by a physician who is specially trained and schooled and has experience in the field. However, there have been instances of minor bleeding where a biopsy was done, or where a polyp was removed; the bleeding is typically minimal and doesn’t usually require additional attention. Occasionally there have been holes or tears in the GI tract lining, otherwise known as a perforation, but it is exceedingly rare. More commonly, patients have an adverse reaction to the sedatives or complications due to existing heart or lung disease.
Upper Endoscopies are known for being very safe, but it is still important to know the warning signs of possible complications. In the event of a developed fever, difficulty swallowing, throat chest or abdominal pain, bleeding, or black stool, contact the center or physician immediately. It is possible for bleeding to occur several days after the procedure. Any concerns should be addressed as soon as possible in order to treat any early signs of issues as a direct result of the procedure.